Sign language care team improved quality of life for elderly people
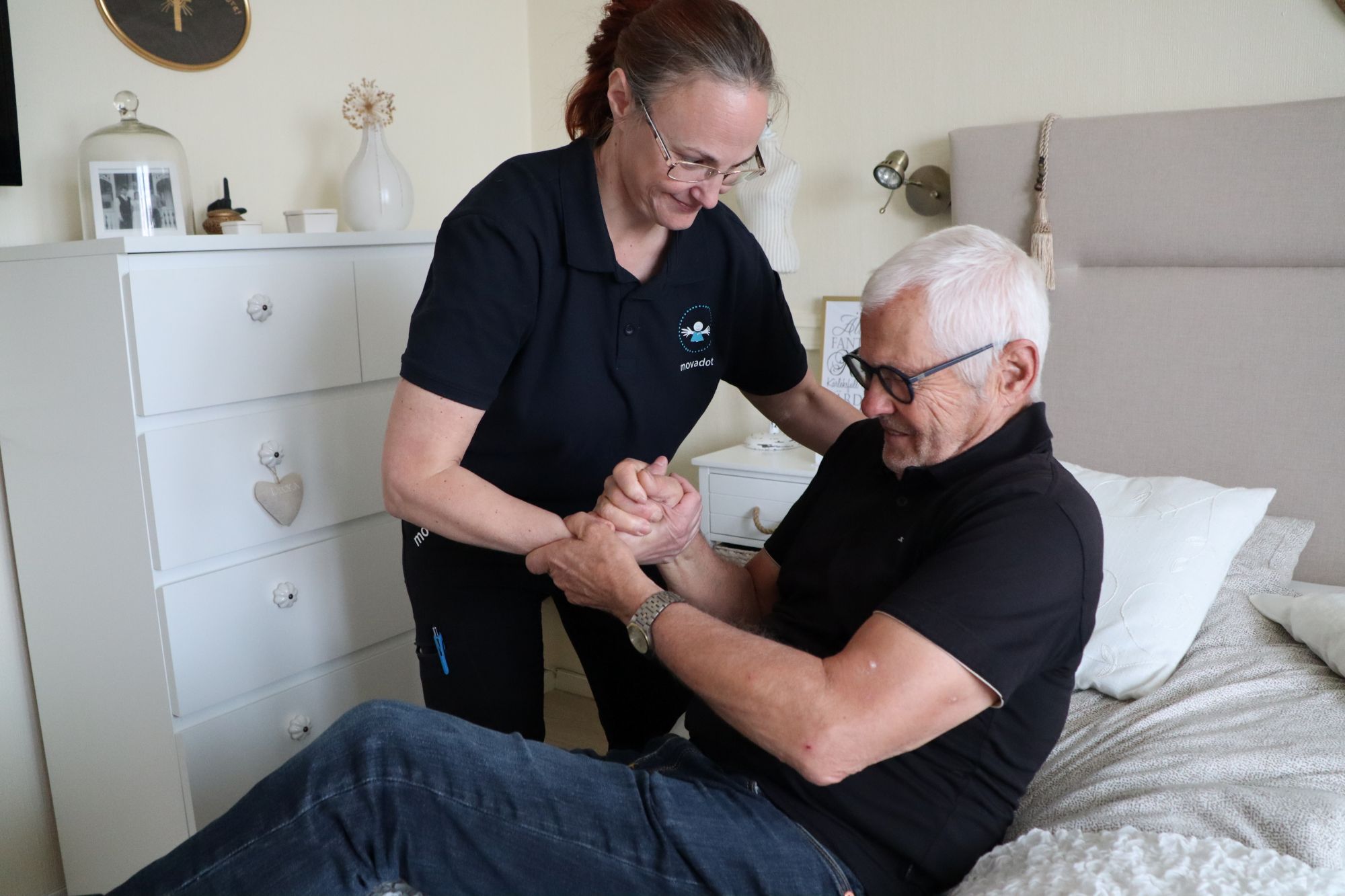
Photo: Sofie Rotstedt, Region Jönköpings län.
Elderly deaf people often face significant barriers in their contact with healthcare and social care services. When staff lack sign language skills, it becomes difficult to understand information, express needs and participate in decisions. A new study led by Sofi Fristedt, associate professor at Jönköping University (JU), shows how a mobile care team made up of deaf nursing assistants can fundamentally improve the situation.
"Our research shows that this approach should not only continue, but should also be scaled up. It's about equal care," says Sofi Fristedt.
The study, conducted by the School of Health and Welfare at JU, is the first in Sweden to examine an initiative of this kind, and it shows how a mobile care team consisting of deaf nursing assistants can change the situation for elderly deaf people for the better. The team, which was put in place by a regional deaf association, visited elderly deaf people in their homes or in residential care and offered support in Swedish sign language. The research team conducted 15 interviews with four participants over a two-year period to map how the support was perceived and what effect it had on everyday life.
Communication in sign language made a significant difference
The study clearly shows that the ability to communicate in sign language was the factor that had the greatest impact. The participants described how previous contact with regular home care services often took place through inadequate lip reading or via notes, methods that were rarely sufficient to express nuanced needs or questions.
"We cannot overstate the importance of older deaf people having access to professional support in their first language. For them, it’s not just about receiving information, but about getting their voice back," says Sofi Fristedt.
Through the team, the elderly were able to have deeper conversations, ask questions, understand written information and make active choices for the first time. The team also helped in dialogue with authorities and healthcare staff, which further strengthened participation.
The mobile team not only performed traditional care tasks such as cleaning, shopping and going for walks but could also assist with activities that otherwise fall outside the scope of ordinary care, such as organising the home, accompanying clients on outdoor activities in nature, helping with hobbies or sitting down for a chat when needed.
The participants explained that this made everyday life both more meaningful and more manageable. Several described how they now actively chose to opt out of parts of the regular home care service in favour of the mobile team.
“For many of the participants, the team became more than just care, it became a social and cultural lifeline,” says Sofi Fristedt.
Psychosocial effects: more joy, security and energy
One of the study's most important conclusions concerns how the support affected the participants' mental well-being. Many described how they felt less lonely, happier and more energetic. They looked forward to the visits and experienced feelings of increased security – at home, in social situations and in contacts with healthcare providers.
Continuity played an important role: the same staff turned up each time, which provided stability and helped build relationships. This was something the participants felt was lacking in regular care.
The researchers believe that the model can be used by several municipalities or regions together, since the target group is small, but the needs are great. Creating truly person-centred care for elderly deaf people requires language skills, cultural understanding and time to build relationships.
